Speak to a doctor, surgeon or nurse and many of them will be able to will tell you about the flight that crashed because the entire crew was focused on a landing gear indicator, or about the jets that collided on the runway because the captain of one overruled the flight engineer and continued with take-off. They will have learned these cautionary tales as part of their training in the arts of communication, decision-making, leadership and cooperation, the so-called soft skills of human factors.
The concept of human factors is widely regarded as aviation’s gift to medicine. The conventional view—backed up by frightening patient harm statistics—is that medicine is the laggard when it comes to human factors. But there is a school of thought that says some corners of medicine have learned valuable lessons to offer back to aviation. Lessons passed from the cockpit to the ground may now need to travel in the other direction.
CASA safety systems inspector, Leanne Findlay, says both aviation and medicine require skilled naturalistic decision-making in a complex environment. Both are subject to time pressures, dynamic situations, and high consequences of errors. And both set great store on experience, which, crudely, is the level of a practitioner’s exposure to adverse conditions.
When the going gets weird: aviation’s safety paradox
Modern air transport accidents are WEIRD, says Patrick Hudson, professor of the human factor in safety at Delft University of Technology in the Netherlands. WEIRD is an acronym, standing for wildly erratic incident, resulting in disaster. The essential weirdness of modern accidents, such as Qantas 32, Air France 447 and, perhaps, Malaysian Airlines 370, is a reflection of the fact that aviation has been spectacularly successful in addressing simpler accident factors.
With 34 million commercial flights in 2015, and no losses of any jet airliners apart from two that were the result of deliberate acts (Germanwings flight 9525 and Metrojet flight 9268), the statistics support his interpretation.
However, Hudson says society’s ‘goalposts have moved’ and no commercial air transport death is seen as acceptable. His concern is that the sorts of higher order thinking, cooperating, communication and decision-making skills, which are the only defence against WEIRD scenarios, are not being taught effectively in aviation.
The problem is the way human factors skills are perceived as ‘soft’, he says. There are no unambiguous right and wrong answers and everyone does human factors in their own way.
‘Performance on hard problems can be assessed objectively, pretty much like maths; performance on soft problems like “What’s going on?” in contrast, is much more subjective, like marking an essay,’ Hudson told the Safeskies conference in Canberra last year.
The result has been stagnation, he says.
‘Modern crew resource management (CRM) training, I am afraid, has all too often become a drill exercise, reduced to the same methodology as technical drills … it doesn’t receive the attention it still needs; in particular in the area of decision-making and handling of emergencies. I am fairly happy about the inter-personal and social issues; it’s what is needed even when those are good that concerns me.
‘People also get taught so that they know what they should do, but what is often missing is the assurance that, after the training, they will actually behave in the best, or at least a good, way.’
Hudson argues that CRM training tends to be limited to teaching the syllabus, assessed by standardised drills because it is hard to ground a pilot for failing an unusual test. ‘But unusual tests are exactly what recent disasters such as AF 447 have provided, where failure was disastrous for more than just the careers of the flight crew.’
Hudson’s concern is that aviation CRM training is clear on what a crew should do, but offers no guidance on how to do it. He finds an example of better practice in medicine.
Trauma medicine, by its very nature, has to deal with emergencies. To do this it has developed a recognised and respected training philosophy.
Advanced trauma life support ([ATLS], also known as emergency management of severe trauma, [EMST]) was developed by a surgeon who was also a private pilot, in response to the chaotic care he received after a crash that killed his wife and injured him and his children.
More than one million doctors and nurses have undergone ATLS training, which emphasises role play in simulated emergencies to develop human factors skills.
Hudson sees ATLS as an example for aviation mainly because of the element of difficulty, stress and realism it brings to an otherwise esoteric subject.
‘They have lectures and discussions too, but most of the time they get out of their chairs and physically practise scenarios, using dummies but also real actors (usually medical students). One comment I have found in ATLS training is that, after the book learning, when they try the first scenario in practice they find just how hard it is to put that knowledge into practice. In the active part of the training all too often things don’t go to plan, just like real life, and they have to find their way out.’
Trauma surgeon, and chairman of the Royal Australasian College of Surgeons EMST group, Dr Scott D’Amours, says EMST/ATLS was developed for doctors who provided trauma care and were expected to manage it as part of their routine jobs but did not have formal training in it.
‘The principle of EMST is that we look for, assess and prioritise for the things that can kill the patient most quickly. It’s distilled to a checklist: airway, breathing circulation, then disability, and exposure—A-B-C-D-E,’ he says.
D’Amours says ATLS/EMST is taught with both classroom and simulation components. ‘We use simulation of resuscitation. On the first day we show them how it works, on the second day they get some practice, and on the third day we examine them.’
Saving Barry—the rise of medical simulation
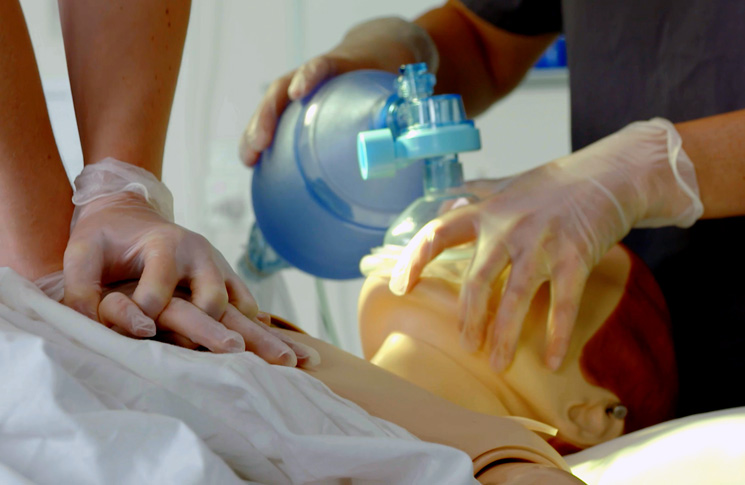
The nurse steps purposefully across the ward and palms a button on the wall, waiting momentarily to be sure the alarm has registered. Within seconds others are in the room. ‘This is Barry, aged 48. I’ve just checked him. He’s not responding, and not breathing. Can you get the bag and mask?’ she says of the patient in the bed. Further conversations take the same terse but calm tone. A junior consultant, looking hardly old enough to be out of high school, let alone medical school, takes charge: ‘Kelly, can you do the chest compressions? Lisa, do the ventilation. I’ll get the defibrillator trolley.’
The team works fast but constantly cross-checks. As the defibrillator comes to full charge, the young doctor makes a final enquiry, to which the answer is ‘still not breathing’. He gives a formal command to stand clear and confirms by looking that the others have done so. They show they are safe by raising both hands. Just as the pads go to Barry’s chest a disembodied voice says, ‘OK, good, can we run through it one more time, please?’
The simulation director emerges from behind a glass wall and with a few polished sentences encourages a reflective discussion by the team of how they performed. It’s a typical day at the Sydney Clinical Skills and Simulation Centre at Royal North Shore Hospital. And Barry is the name of a cardiopulmonary simulation mannequin, under continuous development since 1968.
Medical simulation is both old and new. Physicians have used mannequins for practice and drill for hundreds of years but as with flight simulation, there has been a dramatic increase in realism over the past 20 years. (Tellingly, the Society for Simulation in Healthcare was founded as recently as 2004.)
Modern mannequins can simulate breathing, pulse, pupil response, and pain; and specialised models simulate everything from resuscitation to childbirth. There are mannequins that can be remotely operated over the internet, have lips that turn blue to simulate hypoxia, and specialised anesthesia training mannequins that react to gases and drugs just as a human body would. Over the past two decades the use of simulation has expanded, in parallel with the growth in medicine’s version of CRM, which in the hospital is called crisis response management. CRM emphasises technical and non-technical skills.
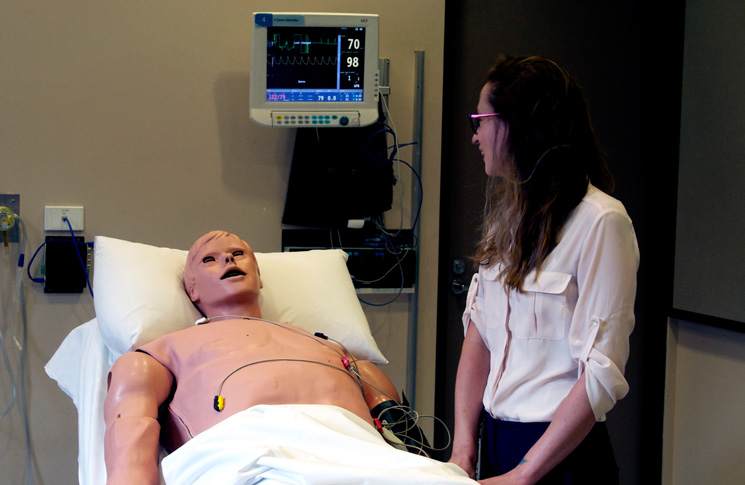
‘Simulation is used from day one as a student and it’s ongoing,’ says the simulation coordinator at Royal North Shore Hospital in Sydney, Stephanie O’Regan.
She says simulation can develop a range of skills, ‘motor skills, how you place things, and also those skills you need to work in an environment when things go wrong: how you talk to one another, how you convey information, how you maintain awareness of what’s happening round you.’
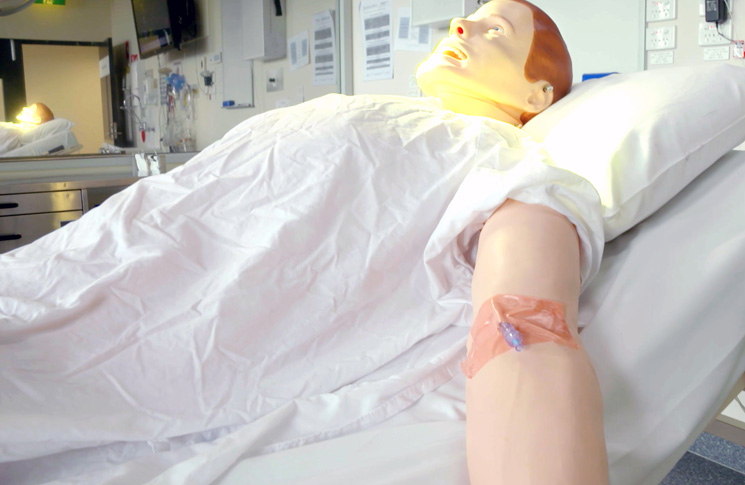
O’Regan says realism has varying degrees of importance for simulation, depending on context.
‘If you’re going to learn how to put a drip in, you don’t need a realistic looking arm but you need something with a realistic feel,’ she says.
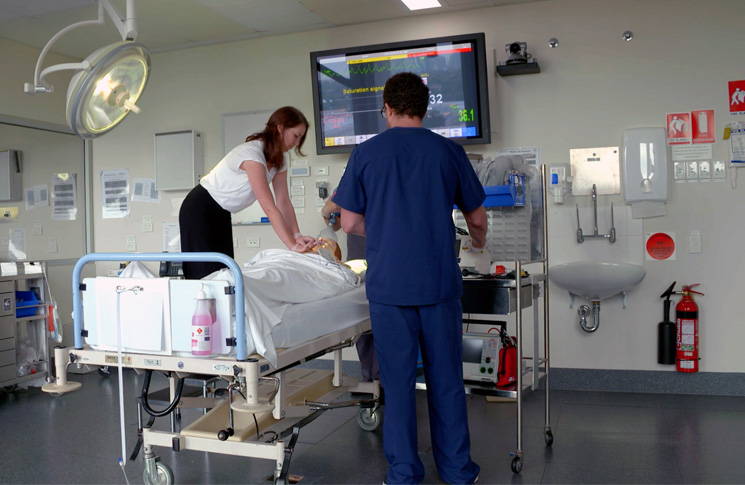
However, realism is important for ‘full-mission rehearsals’ that develop human factors skills. ‘If you are practising an emergency, you want the whole room to feel realistic. It needs to feel real, it needs to look pretty much like your workplace, so people can immerse themselves in the situation and feel the things they would feel in their normal environment.’
Dr Stuart Dilley from St Vincent’s Hospital’s Clinical Education and Simulation Centre, in Melbourne, agrees: ‘There are some things we will teach on relatively low-fidelity, cheap, part-task trainers, before we give them a more immersive simulation with a team, where the task needs to be done under added stress, in conditions of near realism.’
O’Regan says simulation can partly ‘inoculate’ people for frightening and rare events. ‘They run through it once or twice so that if it happens in real life they have an idea what to do, they know what they’re looking for.’
Polishing your act—simulation as drama
In the journal Simulation in Healthcare, Karen Szauter writes, ‘Historically, simulation-based activities have been grouped in two broad categories: model-based simulation (technology-enhanced simulation) and simulation programs employing actual people (simulated or standardised patients or participants).
‘The added benefit blending of technology-based simulations with people (participating in roles from patients or family members to health care providers) is increasingly recognised as a valuable educational tool,’ she writes.
O’Regan describes full-mission medical simulation as a combination of medicine and theatre. ‘There’s a lot of theatre involved. It’s staging, getting the props right and getting the actors right to get the best result possible.’
The lessons learned from full-mission simulation are different, she says.
‘It’s how we function in teams, how we communicate, and how we maintain awareness; how to be a leader; how to be follower; how to communicate appropriately in high-stress, high-consequence situations.’
Dilley says the theatrical element in simulation develops higher order skills that cannot be learned by drill or rote.
‘Your standard Harrison’s medical textbook is about 10 centimetres thick: even then you can’t write every possible scenario,’ he says.
‘But you can write half a dozen scenarios that test leadership skills, teamwork skills, people management and communication skills, which are more generic, and transferable. When it goes pear-shaped with something they haven’t seen before they have these basic principles to fall back on.’
As in live theatre, the audience is part of the performance. Debrief and peer assessment play a large part in an effective simulation says St Vincent’s simulation assistant Matthew Williams. He points out that simulation exercises typically involve 12 participants, with three in the simulator and the other nine watching and waiting their turn. In an hour-long exercise the simulation accounts for 15 minutes. Debrief and discussion accounts for the other 45 minutes.
‘We borrow heavily from theatre,’ Williams says. ‘We invite people to step into the room, we point out the obvious failings of the room, and we invite people to step across. It’s referred to as a “fiction contract”—that you treat it as real, suspend disbelief.’
One of the standing instructions for simulation is that participants who sense the ridiculousness of trying to revive a dummy, for example, keep their doubts to themselves so as not to spoil the exercise for others.
‘What you end up with is a sharing of stories and experience,’ Williams says. ‘And you get a much deeper, richer response. ‘‘When that happened to me,” is often the starting point for a discussion.’
Williams says learning takes place when teams watch each other undergo the simulation. ‘There are times when it’s like the audience in a pantomime,’ he says. ‘They’re pointing at the screen and shouting “what about?” “Watch out!” and “No!”’
Williams says a successful simulation exercise passes the test of good art: ‘it creates response,’ and this response facilitates true learning.
St Vincent’s clinical simulation coordinator Ruth Callander says participants can become deeply involved in a well-run simulation. ‘It can produce strong emotional responses. We had a consultant become very emotional during a death and dying course we ran recently,’ she says.
‘There’s a fine line between intensity and overdoing things, and controlling that is the role of the simulation director.’

All the world’s a stage
Patrick Hudson’s interest in human factors teaching sprang from an uncomfortable realisation: using simple mathematics it is possible to demonstrate that there are millions of possible accident scenarios.
Training for every one of these is obviously out of the question. The requirement then is to develop flexible thinking and skills that will be versatile enough to take on problems that can’t be imagined. Hudson is concerned at ‘the unwillingness of regulators to accept testing situations that cannot be prescribed (and therefore practised) in advance.’
The theatrical method for developing analytical, communication and decision-making skills may have been hiding in plain sight for several years. Charlie Victor Romeo is a play produced by New York avant-garde theatre troupe Collective: Unconscious in 1999 and released as a 3D film in 2014.
It consists of cockpit voice recordings from crashes, re-enacted verbatim, and has been adopted as a training aid by hospitals, university aviation courses and the US Air Force. Co-producer, Patrick Daniels, says ‘People use the examples in the film to analyse how behavior is either good or bad, and they try to teach medical professionals and aviators how to think in terms of working together in a crisis environment.’
In Charlie Victor Romeo the simulated cockpit enters the theatre. What simulation in medical training shows is that there is a case to be made for theatre to enter the simulator.






Comments are closed.